June 16, 2015
New Countdown case study explores how this happened, and why maternal and newborn survival progress is much slower
June 16, 2015
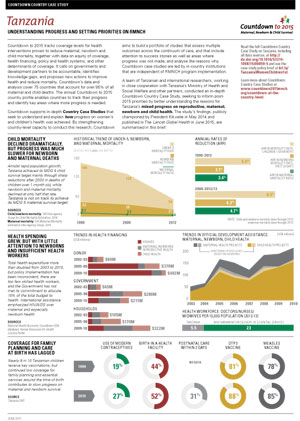
 Tanzania has achieved Millennium Development Goal (MDG) 4 for child survival, yet progress for maternal and newborn survival is off track, according to the Tanzanian Countdown to 2015 Country Case Study, published in The Lancet Global Health on 16th June to mark the Day of the African Child. Simultaneous to the paper’s publication, Countdown has released a one-page Briefing Note that summarizes the study’s key findings in infographic format.
Tanzania has achieved Millennium Development Goal (MDG) 4 for child survival, yet progress for maternal and newborn survival is off track, according to the Tanzanian Countdown to 2015 Country Case Study, published in The Lancet Global Health on 16th June to mark the Day of the African Child. Simultaneous to the paper’s publication, Countdown has released a one-page Briefing Note that summarizes the study’s key findings in infographic format.
This study — one of a series of in-depth case studies that Countdown has supported in Niger, Bangladesh, Peru, and several other countries — collected and analyzed the best available data from 1990 (the MDG baseline) to assess changes in maternal, newborn and child mortality, determinants of this change and who was being left behind. The Tanzania study’s author group includes representatives of a range of key institutions, including the London School of Hygiene & Tropical Medicine, Evidence 4 Action, WHO, UNICEF, the Ifakara Health Institute, University of the Western Cape, Save the Children, and Tanzania’s Ministry of Health and Social Welfare.
Co-author Professor Joy Lawn, a longtime partner and leader in Countdown to 2015, commented, “Across Africa very few countries have achieved these targets, and we commend Tanzania. Many neighboring countries are not on target, and this study advances our understanding of how progress was made, and also what the urgent actions are to make sure women and their babies are not left out of this progress.”
Tanzania has made remarkable progress for reducing child deaths after the first month of life, and this progress increased to over 8% per year during the last decade, almost 50% faster than in the 1990s. This Countdown case study estimated how many lives have been saved and which interventions may have contributed the most, with the most lives saves estimated to be from vaccine (12,500), malaria (9,300) and HIV/AIDS (5,800) programs. Notably, these programs received significantly more donor funding.
Yet progress is about 50% slower for newborn and maternal deaths, and even slower for stillbirths (deaths during the last 3 months of pregnancy). Newborn deaths now account for 40% of child deaths nationally, and the rate of progress since 1990 for has been half that for children after the first month of life. Approximately 3,300 maternal deaths are estimated to have been prevented each year, the majority (70%) associated with skilled care at birth.
Any assessment of progress in Tanzania needs to take account of the doubling of the population during the past two decades, putting huge pressures onto the healthcare system (and other social services such as education), which would need to have doubled in size just to reach the same proportion. However the gap for addressing family planning needs has remained the same for 20 years. While modern contraceptive use has increased even in rural areas, there are two geographical regions (Western and Lake zones) where use remains extremely low.
Improving health services around the time of birth are a key missed opportunity. The study reveals that the rural poor are being left behind, with rural women twice as likely to deliver outside a health facility and three times less likely to have a caesarean, in part related to gaps in access, especially to human resources notably midwives, and to the poor quality of care at birth especially labor and delivery, immediate care after delivery in the these areas.
Dr Neema Rusimabayila, Director of Preventive Services, Ministry of Health and Social Welfare Mainland Tanzania, said, “We can be proud of progress for child survival, but know that more must be done for Tanzania’s mothers and newborns, and that is why we have prioritized these actions in a short-term national plan that we call the Sharpened One Plan. This is already being implemented in the regions and districts. With the national and subnational-levels score cards, we will be able to track progress and improve accountability.”
The authors outline the urgent priorities for Tanzania, as shown in the Sharpened One Plan in order to end preventable maternal, newborn and child deaths by 2030 and contribute to the achievement of the Sustainable Development Goals (SDGs), as follows:
- Address family planning needs especially in regions in the Western and Lake zones, and for adolescents;
- Ensure all women and newborns receive quality care around the time of birth addressing care during labor and delivery, immediate care after delivery and postnatal period, especially close the urban/rural gap; and
- Finish the unfinished agenda for child survival to sustain the gains in MDG 4.
Recommended actions include urgently addressing the health workforce crisis especially midwives in rural areas. The health workforce is at a critical shortage – the minimum recommended health workforce density is 23 health workers per 10,000 people, yet Tanzania has just 5. In addition urgent focus is needed to improve the data to measure progress – for example only 16% of Tanzania’s children get a birth certificate — and use of Information, Communication Technology (ICT) to ensure timely availability data and reporting.
The case study’s authors estimate that approximately 60,000 lives could be saved each year with intensified efforts to achieve universal access to essential health services. This would include the annual prevention of around 22,000 newborn deaths, 23,000 deaths of children aged 1 month – 5 years, 3,600 maternal deaths, and 11,400 stillbirths.
Dr Moke Magoma, evidence advisor of Evidence for Action (E4A) Tanzania, said, “Having a good plan in place is only the first step in saving lives. Evidence must lead to action, especially for the poorest Tanzanians and the marginalised groups. Accountability is essential here, for government, partners, civil society, and the media, communities and individuals – We all must play our part and keep track of the promises and progress made.”
